If her name looks familiar, it’s because Dr. Meagan Peeters-Gebler PT, DPT, CSCS, CMTPT, along with colleague Dr. Brianna Droessler-Aschliman PT, DPT, CMTPT, have been doing a monthly blog with Gennev for several years.
They’ve educated us on pelvic floor issues such as incontinence, prolapse, and sexual function; they’ve taught us about high heels and standing desks; helped us understand and relieve pain and keep our bones strong.
In this video/podcast, Dr. Meagan speaks with Gennev Health Coach Stasi Kasianchuk about pelvic function. What are the pelvic muscles? What do we use them for? How do we keep them strong and fit?
Watch the video of Pelvic health with Dr. Meagan Peeters-Gebler on YouTube. Full transcript is below.
The Path To Better Pelvic Health
Gennev:
Welcome to the Gennev podcast. In this series we talk with the experts about women’s lives and health in menopause. Our mission is to empower you with information that puts you in control of your health. We’re glad you’ve joined us. Let’s get started.
Coach Stasi Kasianchuk:
Today, like we talked about, I want to get your insight as a Doctor of Physical Therapy on pelvic health, pelvic stability. I’ll start off by introducing myself to our audience. So I’m Stasi Kasianchuk, I’m a Gennev menopause coach and I’m also a registered dietitian nutritionist with expertise in sports nutrition and exercise physiology. So with this topic I’ll start it off by saying I have a, I’ll call it somewhat understanding of pelvic health. I know it’s important from my anatomy and physiology classes and previous life as a group exercise instructor and personal trainer. I’m familiar with that musculature, but I know now that there’s been a lot more research and a lot more targeted approaches for pelvic health and stability. And so I’d love for you to just introduce yourself, your role as a Doctor of Physical Therapy, maybe give some insight into what that is in case some of our audience members are not sure of it. And then what is your role specifically in supporting women’s health?
Dr. Meagan Peeters-Gebler:
All right, thank you. My name is Meagan Peeters-Gebler and I am a Doctor of Physical Therapy as well as a postpartum and pregnancy corrective exercise specialist and a certified strength and conditioning specialist. So you know, as a Doctor of Physical Therapy, our introductory education is, is pretty general into the field of women’s health and pelvic health. So most of us who go on to pursue this specific area of study, it’s kind of postgraduate work and continuing education to acquire those skills and knowledge. And it is basically looking at the pelvis as a part of the whole, right. So you know, kind of as, as general PTs, we often look over the fact that it’s muscles, tendons, ligaments, nerves, bones. It is made up of exactly the same stuff that our necks and our backs and our shoulders are. And, and just making sure that we recognize its important role in the musculoskeletal system for pain, and like you alluded to for lumbopelvic stability but then also for continence or keeping, keeping our urine and stool in, and then sexuality. So I’m kind of putting all those pieces together and figuring out how mechanically as PTs we can promote better overall health and function to those, those areas.
Coach Stasi:
Excellent. That’s a great overview and gives us some good things to talk about and to dive deeper in. I would say so as an exercise physiologist and like I said, previous personal trainer and someone that also tries to make exercise a part of my life, in a way, honestly, my goals really are to stay healthy and to have longevity and understanding the learning more about the importance of musculature all over our body and pelvic health has really, as I’ve been in this field a little bit longer, learning more about that. So my general understanding is that the pelvic floor as you plays a role in obviously continence and making sure that urine and stool do stay where they’re supposed to be until we actually move them out on our own planning versus not. And then also from a core stabilization, I mean the pelvis is really close to the low back. It’s the connection to a lower body. So I’ve had an understanding that that strength in that area can also be important for decreasing risk of injury in other areas of the body. I would love for you to just dive into that. Correct me if I’m wrong on some things. And you know, let’s clarify some of this for our listeners.
Dr. Meagan:
Definitely. So I always like to point out that, you know, research has shown that disorders with continence and breathing actually have a higher correlation to low back pain then obesity or inactivity. So I think that is kind of a, a profound, you know, like way of, of really recognizing the importance of the pelvic floor, but then also the respiratory diaphragm as it relates to the pelvic floor in kind of a systemic container pressure management system. Right. We know that, that the pelvic floor, yes, is, is kind of a hammock of muscles that slings across the bottom of the pelvis.
Coach Stasi:
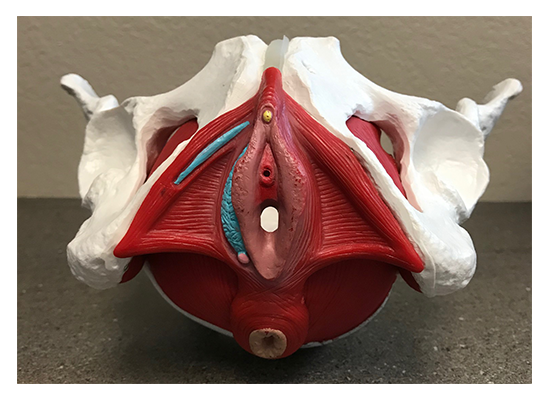
A visual!
Dr. Meagan:
Yeah. So it’s there, it attaches to, you know, the entire pelvis, it attaches to the tailbone and the sacrum. And it really does span and serve as like a structure and a structure to that the whole bottom opening of, of our body. And, and if there’s either weakness or incoordination, there is going to be an inherent vulnerability to everything that is stacked on top of that.
Coach Stasi:
Oh, that’s such a good point. Yeah. And is it possible? I guess what I notice a lot with a lot of the clients I work with through the HealthFix Program is that all of a sudden during menopause, things are just happening all over the place. And, they start to notice things that they may have not noticed before. So, you know, related to pelvic health, maybe all of a sudden there is more incontinence or they’re really wanting to improve sexual function or get their sexual function back. Is it possible, over time because someone may not be aware of this, we may not be working on supporting our pelvic health, then menopause hits with all these other things. And it’s accumulation of not supporting pelvic stability for years that happens at this point? Or is it really something that during menopause, the decrease in estrogen and what’s going on during menopause affects?
Dr. Meagan:
Yeah. You know, I almost so clinically I see it. Plus it’s like the straw that breaks the camel’s back, right: So, you know, gravity and bad habits and posture and life have been like cumulating insults on these poor structures. You know, we also know that the vast majority of women who are verbally taught Kegels are doing them wrong. So so it’s, it’s almost like, yes, we’ve been exposed to all of these challenges. If we’re even worse patients, you know, with without estrogen and without that good blood flow, suddenly these healthy, plump muscles get thin, and fragile and weak, and just the structural integrity automatically diminishes if you do nothing else besides ride it out. So, so wanting, wanting to either prepare before, be actively engaged during and, and figure out continued maintenance from a PT perspective I think is huge to navigate that time.
Coach Stasi:
Yeah, and I would say some of the questions that I get from a lot of the clients I work with, a lot of them are having back pain or knee pain. Are some things there. And I often recommend that they do exercises with a physical therapist, go to see a physical therapist to make sure that they’re doing exercises correctly. And you bring up a good point about the Kegels that most people are doing them wrong. So can you talk a little bit about what you see as maybe some challenges for women and then how you address that? And maybe give us some instructions on what is the correct way to do Kegels, if that’s possible over a podcast.
Dr. Meagan:
Right. Yeah, definitely. So you know, I think what, what we encounter typically in a clinic is that, kind of two diverging paths. One is that women are either squeezing with all their might, kind of everything between their ears and their eyebrows and their knees and their toes, like everything is gripping. And that is just too much that they end up actually generating too much pressure and making their pelvic floor have to work too hard.
And on the flip side, it’s that there’s absolutely no connection. You know, it’s like pelvic floor, what? Is that my anus, is that my, you know, like how do I even feel that, like I don’t feel anything moving. So it’s that women are either excessively connected or totally disconnected to those parts of the body. Usually what we do is we kind of take the approach of helping them find those body parts at the base of their pelvis through the breath. Because when we use the breath, what we can do is we end up tapping into some of the automatic reflexes and just exploiting the physics of how pressure moves through your body as a container to help them hone in on exactly what parts they should be feeling, in which direction, and to what extent.
Coach Stasi:
Oh, interesting. Is that something you could even direct me through right now over the over the podcast? I’ll give it a trial, like, you know what I’m feeling?
Dr. Meagan:
Yeah. So, so kind of the spiel that I like to give is that our body is a container, right? We have air on top in our lungs and in our rib cage. Then we have a diaphragm that separates our air from our guts, then we have our guts. And then we have our pelvic floor, right? And as air moves through our container, the shape of our container should change. And the pressures inside should also change. So as you inhale and you inflate your container, your rib cage should expand in all directions to accommodate that, that added air. Your diaphragm should drop to make more space for air. And in doing so, your guts should bulge out to the front and down to the bottom a little.
So on an inhale you should feel your perineum, your pelvic floor, kind of that space between the vaginal opening and the rectum and the anus drop slightly in response to the fact that air has been added to the system. Okay. On the flip side, when you go to let the air out and exhale, which you’re going to feel is your rib cage shrinks, your diaphragm actually lifts up kind of following the air out of your body. That creates a loop, a little vacuum that pulls your guts up and in as well as your pelvic floor. So we like to get gals kind of rocking and rolling with that breathing rhythm where on the inhale inflate, notice the pressure in the expansion. And then on the exhale, think about gently lifting two beans, right? So think about squeezing around and pulling up and in at the vaginal opening as well as at the anus.
And you want to include, well the front and the back openings because the pelvic floor muscles sling around both of them. Yes. Okay. So you inhale, inflate, feel things descend and then you exhale, lift, gently squeeze and notice that there’s a lifting action that happens.
Coach Stasi:
Wow, that’s incredible. I don’t, I think I’ve ever thought that process through and it’s a good reminder of really that deep belly breath versus the short inhalations that we… myself, I’ll speak for myself to have a tendency to do more often where that is such a valuable benefit. And I actually, I have never heard of that comparison before, so that was really helpful to take that time to really think about where is my pelvic floor, where are those muscles and what are they doing?
Dr. Meagan:
Yeah. Yeah. I tend to also see a lot in the clinic where women have become what we call paradoxical or exactly the opposite because in their brains they want to lift up when they’re inhaling, because they want in in in all to go together, and in doing so they actually manipulate both the diaphragm and the pelvic floor to be coordinated exactly opposite of what we want and it’s this constant then tug of war and the pelvic floor just kind of freaks out and quits either by shutting off and allowing leaks or by spasming and tightening up to try to prevent them. That dysfunction kind of shows up.
Coach Stasi:
Oh, interesting. Yeah, so kind of the extremes that we had for our overachievers out there that they have been doing too much or too hard for for years over time.
Gennev:
You can now manage your menopause with Gennev. We’ve helped thousands of women take control of their health with our team of doctors, coaches and products. Join our membership program called HealthFix and work with one of our menopause coaches on your personalized menopause plan. Learn more at Gennev.com.
Coach Stasi:
Well, and it sounds like there’s opportunities for both sides. There’s prevention. So if women are in perimenopause or even pre-menopause, which I’ll admit, I’m pre-menopause, I’m 36 years old, still menstruating regularly, but it’s, so much of this is important for preparing. So I’m thinking a lot about, I know probably in the next 10 years there’s going to be some changes. And so would you say that doing these types of exercises, being aware of the pelvic floor, even before menopause, or definitely in peri-menopause is beneficial for women’s health?
Dr. Meagan:
Definitely. You know, I think across the whole lifespan, you know, I think, I think this is one of those muscle groups that we just kind of take for granted. You know, until there’s a problem with it, it’s off our radar, you know, and I think there’s a little bit of attention postpartum and then it’s like, unless again, unless it’s causing a major problem, we, it just loses focus. But you know, it’s a muscle. It’s a muscle group, use it or lose it. Right?
So I think by having a, a mindful focused approach on including the pelvic floor in your regular exercise routine, you can definitely help counteract some of the loss of muscle health and function from that reduction in estrogen. So I usually try to get women to the point of you know, if you’re, if you’re following a good exercise program and doing a mix of, you know, strengthening and conditioning if you are breathing correctly, correctly and including your pelvic floor during the task that you’re doing, those count as your daily pelvic floor exercises. You know, not everyone necessarily has to sit and do three minutes of Kegels, driving Kegles, uou know, all of the things that often time, you know, we are led to believe is necessary.
But if you can weave it into your day, all the better. And then you’re also gaining the functional benefit of, of your body learning and knowing how to use your pelvic floor to give you stability when you pick up your grandchild or push the door open or all of those things.
Coach Stasi:
That’s great. That’s great to know. It’s great to know that it doesn’t have to be a separate thing. Cause a lot of the women I work with, it’s, they’re already dealing with a lot. And so adding one more thing, like now you have to do Kegel exercises, even if it is just three minutes can really be another straw that breaks the camel’s back. So that’s helpful to know that recommending just breathing appropriately, which has, benefits in so many other areas too, can help them to target that and just bringing mindfulness and focus to that.
Dr. Meagan:
Yeah, no, don’t get me wrong. You know, if you’re in pelvic PT, you’ll be, you’ll be spending some time doing those specific exercises. But like I said, I like to get gals to that point where it’s just integrated in your day because then it actually happens, then it’s not something you have to remember to do.
Coach Stasi:
Yeah, exactly. Well, let’s talk about that. That’s a great point as well. And this is helpful for me, but if someone is that our listeners are listening to this, maybe thinking, Hmm, should I see a physical therapist for this or should, can I just focus on breathing and be, okay? Where’s the line where it’s like, you know what, having someone that’s watching you, giving you instruction where you have an appointment that you’re going to and potentially could provide additional therapy where, where’s the line? Or how did, how do women decide that?
Dr. Meagan:
So that’s a little tricky, right? I’m a pelvic PT, so I think everyone should come see a pelvic PT. I think that, you know, knowing that so many women are, or doing something just so subtly wrong that can really make or break their success that, you know, even just a single consultation with a pelvic PT can be so tremendously valuable to make sure that you aren’t making matters worse.
You know, I, I see women every single day where there, you know, maybe doing a sneaky breath hold in their Kegel and then they wonder why they are still leaking, when they even tried to do a Kegel you know, as they sneeze, it’s like, well you’re actually holding your breath, which is pushing down and your pelvic floor can’t combat the forces there. So so I think having another set of eyes to give that feedback is, is just, you know, priceless.
You know, public PTs are gaining accessibility. For a long time, you know, we were kind of far and few between, but I do feel like you know, there are some, some good resources out there for people to find pelvic PTs. You know, like our national organization, the American Physical Therapy Association has a website. Like find a PT: you can put in “women’s health and pelvic PT,” put in your zip code or city and it can help you locate someone who has good training and resources as close as possible.
Coach Stasi:
Oh excellent. Thank you for that resource. Cause I think that’s helpful with us working with women all over the country. How they know, okay, you know, if I’m looking for a physical therapist that specializes in this, how do I find them? And that’s also a great point: Knowing to ask it, it sounds like they shouldn’t just go to any PT clinic and say I need physical therapy. They should be saying, I want to work with a physical therapist that has expertise in pelvic health. Is that correct?
Dr. Meagan:
Yes. Yeah. Yeah. you know, we do get exposure in our professional training, but like I mentioned, the vast majority is in kind of that postgraduate, continuing education work.
Coach Stasi:
And can you talk a little bit about that? What makes, what have you done to become an expert in this area? What that additional training looks like? So, you know, it helps our listeners to understand and also to make sure that they aren’t going to someone that perhaps doesn’t have that expertise and potentially do more harm.
Dr. Meagan:
Yeah. So there are, there are various groups that offer continuing education. Most of them provide two to three day courses on the weekend where PTs will attend. And it is learning both the kind of didactic information and in depth learning of anatomy, physiology, what’s normal, what’s abnormal, what’s common and what’s uncommon. That combined with extensive lab practice where these physical therapists are practicing on each other. You know, so we’re learning as a patient, someone is doing these exams or these techniques on another PT so that you, you have that experience and that kind of level of understanding to know what, what the person on the table is also going through as you’re providing the services. You know, and, and typically it is then a sequence of courses that most people will end up going through depending upon their interests. You know, if they have more interest in bowel function or dysfunction, pregnancy, postpartum care, pelvic health but, and even in the introductory classes the therapists are going to be exposed to treating urinary incontinence, bowel incontinence, pelvic pain, painful intercourse. All of the things that we, we tend to see women in the clinic for.
Coach Stasi:
Okay. Yeah. So, and, and it sounds like there might be specific approaches for each of those things. So it’s not just a blanket approach for pelvic health. It’s what is your specific concern and here’s the approach for you.
Dr. Meagan
Definitely. Definitely. Yeah. Yeah, yeah. I was going to circle back to what you were saying about knowing if you need a pelvic PT within the last question. And as I was listing those things off, I think that’s, that’s kind of a nice, nice, way to put it on the radar is if you’re leaking anything, out of your vagina or your anus, involuntarily, that’s not normal. And that’s not okay. You know, it may be common and it may be brushed off because of, you know, whatever reason your mom or grandma may have told you. But absolutely there are things that can be done about it that are conservative and quite effective. If you’re having any pain, painful gynecological exams, painful wiping you know, with bowel movements or after urinating, any kind of painful vaginal penetration for intercourse. That should not hurt. And those are also indications that finding a PT you know, as well as working with your, your medical, other medical providers, but definitely things that, that pelvic PTs treat, I think are good to have, good to have on the radar and seek, seek more help.
Coach Stasi:
Yeah, absolutely. And I appreciate you listening out those symptoms because you make a good point. A lot of times, and I see this in a lot our, our Facebook group and when women are talking with each other, they have great community support, but sometimes when everyone in the community is experiencing pain and incontinence, they normalize it. And while it may be, I don’t, I don’t want to say no, I hesitate to use the term normal, maybe common, like you said, during this time of life. And, but it does attention and it doesn’t have to be the normal. It shouldn’t and it isn’t normal. And really does deserve treatment and there’s treatments out there and there’s no shame in it. You know, I think that’s the other part. Sometimes women when I’m talking with them may feel a little hesitant to talk about things that are going on in that area. But it’s important to know that’s a really important part of health and not to feel shame and to know that they can get support.
Dr. Meagan:
Most definitely. Yeah. Yeah. Most of the women that I end up seeing and talking to in the clinic tell me, Oh my gosh, I wish I would’ve known this five, 10, 20 years ago. You know, it’s, it’s again, I think it’s gaining you know, its ability to be talked about more comfortably and knowledge is power. But yeah, you’re right. It still is something that for some reason women are felt to, to feel, you know, some, some personal level of shame about, but should not.
Coach Stasi:
No. And that’s where we’re hoping here at Gennev to kind of change that perception of menopause, this time of life, and really provide the resources that are out there. And based on what you said, it sounds like most women, if not all, should have a pelvic floor PT on their healthcare team or on their menopause support team during this time in their life. I mean, it’s putting the tool in the toolbox to really help them thrive.
Dr. Meagan:
Yes, most definitely.
Coach Stasi:
Excellent. Well, I really appreciate your time today. Is there anything else that you want to add or last tips or points? And give your clinic information and location for any listeners that may be near you just to finish up with.
Dr. Meagan:
Yeah, I mean, I think you know, thank you for having me. I think it’s just awesome that we’re getting the word out and, you know, like I said, knowledge is power and, and knowing that there’s hope and that it doesn’t mean that you have jump on a medication. It doesn’t mean you have to jump to surgery. You know, and there there’s always the potential to make these even slight improvements and, and it’s not, it’s not terribly hard work to do once, once you get committed to it. It’s just a lot of, a lot of changing and bringing things to awareness that can have pretty profound positive impacts on people’s lives.
I practice out of Orthopedic and Spine Therapy. We are a private practice in Wisconsin in the Appleton, Wisconsin area and we have clinics kind of scattered throughout the state but pretty much focused in the Fox Valley area.
Coach Stasi:
Okay, excellent. Well good information for our listeners to locate you or certainly you gave them the information and that was the what was the, the organization is the, the American Physical Therapy Association?
Dr. Meagan:
Yup. APTA.
Here’s to better pelvic health and wellness
Coach Stasi:
Okay, excellent. And you can go on there, put in your zip code and then specifically look up women’s health and pelvic health to find someone that is trained in that.
All right, well just to finish up on my end, I do want to put a plug out there for our HealthFix program. I am a menopause coach as I mentioned in the beginning working with that program. And having that membership, it’s a subscription based membership, you get the opportunity to work with someone like myself and talk with them out through calls as well as have supported accountability between those calls. And so it can be an opportunity as well if you’re thinking, I don’t know if I should go see a pelvic PT even though I think after this we all should, but if you have questions about that or just questions about any symptoms you’re experiencing during menopause, signing up for the HealthFix program gives you the opportunity to have some of those questions answered, provide resources, information and support around finding what the next steps are. Perhaps it’s finding that physical therapist in your area or perhaps it’s just figuring out what that next step is for you, whether it be pelvic health or other menopause symptoms. So sign up for that HealthFix program and I hope to be working with more of you that are listening to this podcast today. So thanks very much Meagan, and I hope you have a great rest of your day and I’m sure we’ll collaborate again soon.
Dr. Meagan:
Wonderful. I look forward to it.
Coach Stasi:
All right, take care.
Dr. Meagan:
Thank you.
Gennev:
Thank you. Thank you for listening to this episode of the Gennev podcast. Remember, you can subscribe on iTunes, Google play, Spotify, and just about anywhere you get your podcasts. Gennev is your online destination for menopause, doctors, coaches, products, and education. You can find us at Gennev.com. Thanks for joining.
Learn more from Coach Stasi Kasianchuk and Dr. Meagan Peeters-Gebler by searching on their names on this site.
If you have issues with your pelvic floor or have improved your pelvic health, we’d love for you to talk with us about it. Please join us on the Gennev Community forums!
According to research by Strava, most of us have caved on our New Year’s resolutions by (wait for it)”¦ January 12.
To which we say, “shrug.”
We’re not huge fans of NY resolutions around here, preferring instead to help women achieve their best health all year long. But if you want to get back on track, or if you’re struggling to stay resolved, our awesome DPTs (Doctors of Physical Therapy) have some tips that might help you in your efforts.
Here’s what we learned from Dr. Meagan Peeters-Gebler of Orthopedic & Spine Therapy and Dr. Brianna Droessler-Aschliman from Missoula Bone & Joint about staying motivated and safe when you start or ramp up your better-health routine.
Why do we quit to revitalize our life fitness and how can we carry on?
Our reasons for not sticking with our health goals are probably as varied as we are, but Bri and Meagan do note some trends. Since forewarned is forearmed”¦
One: Unexpected results like muscle soreness, fatigue, pain
We all know exercise can hurt, but what we may not expect is how much it can ache and how long the hurt can last. If you go all-out on January 2, you may be surprised how lousy you feel on January 4.
Solution: Bri suggests you work with a coach, PT, or trainer at your gym to ramp up your efforts slowly and appropriately. Know and be honest with yourself as if hurting is likely to make you quit, create a plan that will minimize the ache. Even a small improvement to your fitness is vastly better than none at all.
Are you experiencing joint pain or arthritis and not sure what to do? Check out our blog with Orthopaedic Surgeon Dr. Darcy Foral.
Two: Poor training
A couple weeks in, poor training is biting us in the backside. At about this mark, says Meagan, if we’ve been doing a daily challenge like an ab workout, the repetitive motion and any poor form is really starting to show up as back pain or another overuse injury.
Solution: Daily challenges don’t take into account our bodies’ needs for rest and varied motion. Anything that has you doing the same pattern of movement day after day is probably not a great idea. Meagan says you can make it safer by (a) checking your form with a health/fitness professional, (b) mixing it up so you’re not doing the same movements every day as maybe alternate with an exercise that targets another part of your body, and (c) taking rest days.
A month of squats can be really hard on your knees and pelvic floor; squats done properly and mixed in with cycling, swimming, walking, and rest can be really beneficial.
Three: Inexperience
Either we push too hard and hurt ourselves, or we don’t know our body well enough to judge if a pain is normal and OK, so we quit to be on the safe side. Gyms fill up in early January, Bri tells us; physical therapy appointment slots fill up the rest of the month.
Solution: First a caveat: Every body is different, so these are just general guidelines to consider. If you’re hurting and you’re concerned about it, by all means, see a doc or PT for a diagnosis and recovery plan.
According to Meagan, if a pain is so localized that you can trigger it by pushing your finger on a certain spot, and The Spot comes back every time you do an activity, that’s a big red flag. Stop doing the thing that hurts and give your body time to recover or see a doc. If the ache moves around or comes and goes or can be covered by your palm (as opposed to a finger), it’s less likely to be urgent or acute.
Bri adds, sharp pains or pains that cause you to compensate by shifting your form are definitely signs your body wants you to stop. If your Achilles tendon hurts and you start favoring that side, you could set off an unhealthy chain reaction where now your knee hurts, your hip hurts, your IT bands ache, your lower back is sore”¦ you see where we’re going with this. Stop. See a doc. Rest.
One way to know if your form or gait is off is to check in with a work out or running partner, Meagan says. Anyone who’s exercised with a buddy knows you start to recognize your partner’s “natural” form, often without being consciously aware of it. If your gym friend or running buddy asks if you’re hurt or limping or otherwise doing something funny, listen. They may be picking up on cues you’re missing. And if it’s obvious to the non-professional, you really need to pay attention.
If pain starts with the activity and intensifies as you continue, and if it hurts worse at the end than at the start, that’s a clue that tomorrow is a rest day. Pain that is with you at the start and lessens or goes away completely is probably OK to power through, as long as it’s not severe, localized, or changing your form.
Four: unrealistic expectations
Pair crazy expectations with someone who’s just starting to get to know their body’s abilities and limits, and you can be in for some disappointment. As Bri tells us from her experience with clients, your body may hurt more or your performance may improve more slowly than you expected, or you may be plateauing in terms of weight management. Any or all of these can cause us to throw up our hands and head back to the couch.
Solution: It’s OK to re-evaluate your goals, says Meagan. If you decided to run a marathon in 2019, maybe reassess and see if a half-marathon or sprint triathlon is easier to stick with. That’s not to say you couldn’t run a marathon in 2019, just that the lesser pressure of a different goal might make it easier to stay motivated. When we set resolutions, we can get compulsive about staying on track. Allowing yourself permission to reassess may be the difference between healthy achievement of that new goal and “failure” and/or injury with the old.
Blame social media for some of this tendency to be unrealistic, Bri says. Your friend’s Facebook posts about getting fit may make it look like she went from unhealthy to Olympic while hardly breaking a sweat, but you may not be seeing the steps between. In addition, your body is uniquely, wonderfully yours, and your fitness journey will be too. Applaud your friend’s achievements, but don’t compare them with your own.
Five: underestimating the process
There’s a tendency among those new to fitness to believe that it’s a constant, steady progression, and each day you’ll be better than the previous day. That’s just not true, but that myth is often why it can be hard for some new athletes to take rest days.
Solution: If you’re new to the fitness thing or just adding a new activity, talk with someone who’s been doing it a while. Ask them about their experience so you get a better idea of what’s involved. We do this for new employees when we “onboard” them, right? No one expects you to know everything your first day at work. Have equal patience with yourself your first day at a new activity. Also, having a buddy to check in with and stay accountable to is a great way to stay motivated.
And rest. “You’ll be a better, stronger, faster athlete and able to perform longer, if you recover between workouts,” Meagan says. “There’s a reason your fitness watch or app has built-in recovery periods of 24 hours or 12 hours or whatever,” Bri says. “Follow it.”
Be patient and understand that bodies are bodies and you’ll have good days and bad days. Don’t let a belief that every workout should be better than the one before be a reason that you quit or push yourself to the point of injury.
This is particularly important for women in midlife. Your body may not respond to changes as quickly or dramatically as it did when you were younger, and energy levels during the perimenopause/menopause years can be really low. Hormone fluctuations, fatigue, interrupted sleep, greater stress can all make exercise really tough. However, most women find that this is temporary (though “temporary” can mean months or years), and it gets easier when hormones level out on the other side.
Six: too few rewards for the effort
The numbers on the scale aren’t moving the right direction. The tape measure isn’t showing the anticipated improvement. Your clothes fit the same, no one’s mentioned your change or glow or new found energy. So what’s the point of all this work?
Solution: redefine “rewards.” First, understand that while change may not be happening on the outside, it almost certainly is happening on the inside. Muscles are getting stronger, your heart is getting healthier, maybe blood sugar levels are evening out, your lungs and brain and endurance and immune system are all seeing benefits. The change may be incremental, so small and slow you don’t notice, but suddenly you’re not out of breath from taking the stairs or you’re sleeping a bit better. Appreciate that even if you can’t yet do more reps or lift heavier weights or go to a smaller size pair of jeans
And reward yourself. As Meagan says, celebrate your accomplishments. You’ve made it a month! Buy yourself a new pair of really good socks or a better sports bra or a new swimsuit. Post a note on your mirror congratulating yourself for sticking with it this long.
If you’ve dropped your new fitness routine, no worries. You didn’t “fail.” “Respecting your body isn’t failing or quitting or being lazy,” says Bri. “You took a few days off to rest and re-evaluate, and now you’re ready to start again.”
As Meagan says, the real achievement is in balancing your approach so you can continue staying active for the long term. Staying realistic, seeking help when you need it, and resting when rest is called for can all help you get past January 12 (or Valentine’s Day or spring break or swimsuit season) and on the path to life-long fitness.
How are you doing with your resolutions or your general fitness goals? We’d love to hear your story and solutions, so please share with us by commenting here, or joining the conversation in our community forums. You can also reach out to us on Gennev’s public Facebook page or in our closed Facebook group.
Hey, SuperGal, before you head out on that bike ride or hike or claim your spot in spin class, have you done what you need to do to protect your body?
Yes, exercise is great for you as for your heart and lungs, your stress levels, your bones, your brain, ALL THE THINGS as but friction, moisture, and pressure in the wrong time, place, and amount can all derail your efforts to be healthier.
To learn more about what bugs us when we’re trying to get fit, we talked to our genius PTs, Meagan and Brianna.
The problem with friction
When skin rubs on skin or skin rubs on something that doesn’t slide very well, you can end up with some nasty chafing. Ask any athlete who whips off her sports bra and leaps into the shower, only to find when the water hits her that her bra has been rubbing her raw for the past couple of hours. There’s usually some shouting.
Friction not only hurts, it can leave us vulnerable to infection, so let’s talk about how to avoid it.
Gone are the days of cotton tees and sweat pants for exercise. Love it or hate it, our PTs tell us, Spandex and other slide-y fabrics are much better choices.
If you’re a biker, Meagan says, invest in a good pair of bike shorts that grip tightly around your thighs, yet move with you. These slide easily over your bike seat, which reduces friction. This is especially important if you’re generating a lot of sweat and spending a lot of time in the saddle.
Chamois (pronounced “sham-ee”) creams and lotions also reduce the skin-on-skin and skin-on-fabric resistance. Apply liberally, Meagan says, on the outside of any parts that get involved, including the external girl bits like the labia minora and majora. Also get the inside of the thighs, any creases or folds in the skin, anywhere your clothes rub repeatedly. “Everything needs to have the ability to slide and glide on itself rather than create friction and hot spots,” says Meagan. Oh, and do not wear underwear under your bike shorts as that nullifies the benefit.
Hint: if it burns when you urinate after exercise, you probably need more help with friction. “The acidity of urine flowing over the skin “in the neighborhood’ causes that pain and burning and indicates points of chafing or friction. This is potentially a risk for infection, so note the spots that burn for chamois cream next time.”
According to Bri, clothing choices aren’t just for bikers. Runners, walkers, and hikers may find that compression shorts reduce unwanted friction. You can wear your Spandex under other clothing, if you don’t feel comfortable with the skin-tight look.
Runners can tell you about the wonders of Body Glide and other friction aids: these usually come in a stick like deodorant and can be rubbed on all the spots where you normally chafe, like under bras, between thighs, around toes, and on the bottoms of your feet. They last a long time (which is why many athletes prefer it to Vaseline) and can be reapplied as necessary.
Pressure and exercise
Friction isn’t the only cause of discomfort; pressure in the wrong places can be painful and lead to more serious damage.
What’s the problem with pressure? Compression in the wrong spot during exercise can reduce proper blood flow, Bri says. If your toes go numb during running or biking, that’s a good indicator that there’s pressure somewhere that shouldn’t be.
And pressure doesn’t just affect a single area. Discomfort from pressure may make you change your posture as you exercise, and getting out of proper alignment can set off a chain of painful issues.
“Pressure is another reason to invest in a good pair of bike shorts,” Meagan tells us. “They come with what’s called a chamois, which is like a big pad sewn into the crotch. It provides a cushion and absorbs friction. You want your saddle to be hard and rigid to support your pelvis, but that can be hard on the bony spots.” With a chamois built in, the bike shorts provide the cushion so the seat doesn’t have to.
Also, Meagan says, be sure your saddle fits you right. It should fit the shape of your pelvis so you’re taking the pressure on your “sit bones.” Those really big, thickly cushioned seats might look comfy for your tush, but in fact, they can make things worse by allowing too much sliding around. Not only does that cause more friction, it also reduces your efficiency as a cyclist.
Another way to fix pressure problems is to make sure your bike is fitted correctly. A good bike shop can make adjustments so your seat is the right height, the handlebars are in the correct position, the length of the bike is good for you, etc. This can make you a more efficient and powerful biker, but even more, it can help you be more comfortable and avoid pressure problems.
You want your bike seat to be level or 2 as 3° “nose down,” Meagan tells us. If it’s tilted too far forward, you’ll slide down and off, and your arms will be doing too much work to keep you in place. If it’s tilted too far back, you’ll be putting a ton of pressure on your pelvic floor muscles and tail bone, and that’s not where you want it.
The shape of your saddle should fit your “sit bones” so you’re resting on your skeleton, not counting on the hammock of pelvic floor muscles. If you sit on a hard chair, you can feel the bones you want to use, Bri says; move around until the pressure is in the right place.
Your insurance may even pay for you to get your bike professionally fitted by a physical therapist, which both of our PTs vigorously recommend. “It’s a good, proactive measure,” Bri says. “Especially if you’re going on long rides or you’re bike commuting more than a couple of times a week.”
What are you avoiding? Spending too much time on a bike that doesn’t fit can cause neck and shoulder pain, headaches, numbness in your hands from taking too much of the pressure there, numbness in your feet, tailbone or lower back pain, knee pain, possibly even carpal tunnel syndrome (PS get bike gloves if this is a risk factor for you). Some women even complain about numbness in their intimate areas.
And, Meagan adds, if you have surgery or take time off, or if you’re ramping up your training, consider that a cue to check your bike fit, especially if it’s been a couple of years.
Incidentally, everything we’re telling you here also applies to spin class. Just because your bike isn’t going anywhere doesn’t mean you’re off the hook for pressure, friction, etc. Bri suggests you spend time getting a spin bike to fit you perfectly, then record all the relevant numbers and measurements for next time.
Pressure as from the inside
Another thing you really want to beware of is any pressure that’s coming from the inside that shouldn’t.
Says Brianna, “If you’re experiencing heaviness in the pelvic floor or chafing at the vaginal opening, that can be a warning of early prolapse at the anterior or posterior vaginal wall. You should stop the exercise and get to a doctor or physical therapist to get equipped with a pessary or another device to support the vaginal wall and prevent chafing.”
For runners, Meagan says, “If you feel like your tampon might fall out while you’re running, that can be a clue that there’s a prolapse happening, so you want to get that checked out. Also, a menstrual cup can help with internal pelvic health during activity. They’re made of silicone or other rigid materials that slide and glide rather than absorb and cling and create friction like a tampon.”
Moisture as not always a good thing
“Moist” is no one’s favorite word, and there’s a reason for that: a lot of the time, it’s not doing your body any favors. Bacteria loves a good moist place to hang out and cause trouble, so it’s best not to give it the opportunity.
When it comes to exercise, wicking fabrics are the bomb. They may be more expensive, but it’s worth investing in a few good pieces, Bri says. Get a couple of good sports bras, shorts, shirts, socks. If you treat them right, they’ll last a long time and save you a lot of annoyance.
And finally, while you may want to spend all day in your bike shorts (HA!), resist the temptation. Sweaty moisture isn’t great for your private areas.
“Practice good hygiene after exercise,” Bri advises. “Don’t sit in your exercise clothes. Get a shower if you can, but at least wash with warm water, no soap, no scrubbing. If you’re really pressed for time, find some wipes that are OK for that area that can cleanse sweat and get rid of bacteria.”
Let’s face it, 50 isn’t what it used to be (and that’s a good thing). Many of us are staying physically active well into our middle years and beyond. To keep enjoying exercise, be sure you’re protecting your body from little irritations that can turn into bigger problems.
How do you protect your body during exercise? Have you gotten good (or terrible) advice you’d like to share with the class? Please feel free to share with the community by leaving us a comment below, or talking to us on our Facebook page or in Midlife & Menopause Solutions, our closed Facebook group.
Health Coaches are a vital link in connecting women with the care they need to take control of their menopause. Gennev Women’s Health Coaches are Registered Dietitian Nutritionists (RDNs) who, in addition to their extensive nutrition training and experience, have been trained specifically in supporting women during menopause. They provide support, recommendations, resources, and accountability to help you navigate menopause and thrive along the way.
We sat down with Gennev’s Director of Health Coaching and Dietitian, Stasi Kasianchuk to gain an insider’s perspective on being a health coach, and how they offer much needed support to women in managing their menopause.
How did you get started in health coaching?
Through my own interests and enjoyment in nutrition and exercise I have come to learn how this can help me feel my best and wanted to share this with others. Through continued education and training as a dietitian in behavior change science I have learned approaches that I use to support my clients in finding the habits and practices that are accessible and realistic for them to implement to feel their best. Throughout my career I have come to learn more about other aspects of our lifestyle, in addition to exercise and nutrition, that impact our quality of life such as sleep and stress management. Integrating these things all together I can support women holistically.
What do you find most rewarding in your work?
Working with and supporting amazing women who, no matter how bad their menopause symptoms, are showing up to learn, willing to be vulnerable, and embrace their beautiful, changing bodies. This is by no means easy. In a society that does not value age, especially in women, it can be hard and uncomfortable to have conversations about menopause. However, we need to have these conversations to support future generations of women. My clients are a part of this change and I love being part of this movement. There is work to be done and the future is bright.
Why should someone consider working with a health coach?
Our health coaches are dietitians who use a supportive and compassionate approach personalized to our client’s needs. Menopause can create uncertainty and isolation. Working with a Gennev coach you have a knowledgeable expert that can answer questions to mitigate uncertainty and provide support. Most importantly, we will always remind you that you are not alone and menopause isn’t forever.
What advice can you offer for someone preparing for their first session?
Calls with your coach are opportunities for you to share your story. It can be scary at first, but know that there is no “wrong way” to do it. It can be helpful to have your main questions, concerns, and primary symptoms causing disruption to your life written down to refer to. If you have questions about supplements have these near you, so you can answer questions about brand, dose, and ingredients.
Are there any themes you have seen recently in your work with Gennev members?
Focusing on more pleasure, joy, and fun has been a theme with several clients recently. While this may differ from what they found pleasure in five or ten years ago, I find that women really benefit from exploring this to learn what joy is for them now. Once they do, and start implementing these things more often, there is a certain freedom and liberation that can occur. When we center on joy in our lives, menopause symptoms aren’t quite as all-encompassing anymore.
What is your personal message to women about the menopause experience?
For too long menopause has been disregarded and women have suffered in silence. This needs to change. We have an opportunity to reclaim this time of life for women to be one of celebration and opportunity rather than doom and gloom. That’s not to say that every day will be bliss and when it’s not, pretend it is. Instead, it’s an invitation to start the conversation, acknowledge the discomfort, and be open to exploring the possibility that there is more celebrating to do.
Schedule a Health Coach Consultation to create your personal plan to take control of your menopause.
About Stasi Kasianchuk
As a sports dietitian and exercise physiologist Stasi approaches her work with her clients through the lens of optimizing performance by supporting and working with an individual’s physiology. Having worked with a variety of clients over the past decade including collegiate and elite athletes to now working with peri/post-menopausal women, she has come to realize that everyone wants to optimize their performance in life. Recognizing that this often looks different for each individual, Stasi uses a personalized approach to help women feel their best. Outside of work Stasi enjoys trail running, swimming, weightlifting, yoga, group exercise classes, and biking; weekly trips to her local farmers market; cooking at home and dining out with her partner; and walks with her dog, Plinko.
Menopause bloat happens. Gas during perimenopause and menopause is common, uncomfortable, and embarrassing. Most women report it as a feeling of tightness or fullness in the abdomen, sometimes painful, always uncomfortable. Some women have it only occasionally or after eating certain foods or at different points in their cycle. Others will have it daily, starting the morning with a flat stomach that gets progressively more bloated throughout the day.
What causes bloating during menopause?
Menopause bloat generally has two causes: excess air or excess water and sometimes both at once. Women may experience an uptick in burping and flatulence. That extra air in your stomach and gastrointestinal tract is either swallowed or created by the fermentation of food in your stomach. There are a few culprits; some hormonal, some lifestyle.
1. Digestion – Gas can result from a general slowing of your digestion and many menopausal women experience constipation during this time for the same reason. This slowing means food has time to ferment in the digestive tract before it’s expelled from the body.
2. Diet – Many women experience weight gain in menopause and so switch their diet to include more fruits and veggies. These can cause gas, certainly at first, before the body adapts to the increase in fiber.
3. Air – Often women experiencing menopausal dry mouth or weight gain start chewing more gum. The artificial sweeteners in sugar-free gums can cause some women stomach problems, and the extra air you swallow as you chew will find its own way back out. Fizzy drinks like sodas or carbonated water can also increase the air in your gut, as can smoking. Yet another reason to quit if you can!
4. Eating habits – At this busy time of life when you may have to grab meals on the go, you may be eating too much or too quickly. Smaller meals enjoyed at a reasonable pace will result in less buildup of food (and therefore gas) in your digestive system.
5. Stress – Stress takes a toll on everything, including digestion. When bad enough, it can slow your digestive system and contribute to bloating, gas, and discomfort.
6. Flora and the microbiome – Menopause can prompt changes in the bacteria of your gut and lead to less diversity in your microbiome, affecting the flora that help break down your food.
Menopause bloating remedies: how can you reduce the gas?
Here are six things you can do to help lessen the gas and the bloat.
Chew. A lot. Chewing prompts your stomach to ramp up production of digestive enzymes so it’s ready to start digesting as soon as the food splashes down, so to speak. It also slows you down if you tend to eat too fast, and it may encourage you to eat less if you get bored with chewing each mouthful 20 times.
Hydrate. There is a persistent belief out there that drinking too much liquid with a meal dilutes digestive juices and makes them less effective. There’s no real science to support this notion. The stomach is able to adapt to the content of meals, including water intake, and in fact, water may help the digestive process operate more smoothly.
Exercise. One of the most natural menopause treatment options is exercise. Exercise can reduce stress and improve digestion, so keep moving so that everything, well, keeps moving.
Eat well. Many healthy foods can contribute to bloating: beans, broccoli, pears, and whole-wheat bread among them. Try cutting way back on the foods that cause you the most problems, then slowly reintroduce them one at a time. This may help you tolerate them better. Fried and fatty foods can cause additional digestive problems, says Nature’s Intentions Naturopathic Clinic, so limit those. If you think your gut flora may be compromised, pre- and probiotics can help. Eat slowly and try to eat when you’re not under stress.
Know your triggers. Many women report issues with dairy, gluten, refined sugar, and artificial sweeteners, so test your tolerance and eat accordingly. We can become more sensitive to foods as we age, so don’t assume something you ate safely and in great quantity as a youngster will be as well tolerated now.
Try peppermint tea. Peppermint is an effective, time-honored digestive aid. Plus it tastes really good. Caution – If you’re prone to heartburn, go easy on the peppermint.
What else could cause the gas?
Gas and menopause bloat can be caused by other health concerns, so be sure to talk with your doctor if the development of gas is sudden, painful, extreme, comes with weight loss, diarrhea or constipation, and/or is disrupting your life.
Other possible causes include:
SIBO – A too-high concentration of bacteria in the small intestine can be the underlying cause for many digestive issues. A breath test can help you determine if this is causing your digestive issues.
IBS – “Irritable bowel syndrome” refers to a group of symptoms that generally cause abdominal pain and changes in bowel movements.
GERD or “gastroesophageal reflux disease” is a condition in which the stomach contents flow backward up the esophagus. Celiac disease is an autoimmune disorder in which the presence of gluten causes the body to attack its own small intestine. Subsequent damage to the villi, the lining of the small intestine, can keep nutrients from being absorbed correctly.
While a little extra intestinal gas may not be detrimental to your health, it can disrupt your work and social life. If you’re dealing with digestive issues, check with a doctor, consider keeping a food journal to help you track triggers, and try to maintain a sense of humor. And maybe get a dog. You can always blame it on the dog.
We can help you find relief from menopause bloat
- Meet with a Gennev clinician – our menopause specialists can help you understand fluctuations in your hormones as they relate to changes in your digestive system as well as any other symptoms you may experience, and provide a personalized treatment plan. Registered Dietitian Nutritionists can help you take a close look at your dietary, exercise, sleep, and lifestyle habits, and come up with customized solutions for your health needs and goals during menopause.
The information on the Gennev site is never meant to replace the care of a qualified medical professional. Hormonal shifts throughout menopause can prompt a lot of changes in your body, and simply assuming something is “just menopause” can leave you vulnerable to other possible causes. Always consult with your physician or schedule an appointment with one of Gennev’s telemedicine doctors before beginning any new treatment or therapy.
If you were a child in the 70s or 80s, chances are you’ve heard of or experienced the Clean Plate Club. You know the one, where you are expected to eat every last morsel of food on your plate because there are starving children in the world who have nothing to eat.
My personal version of this was a face-off against ten lonely, shriveled, tasteless lima beans. My parents made me sit at the table for HOURS after dinner ended until I finished every last lick of limas.
I have wonderful parents, but this was such a horrid experience for me that I never let them live it down, AND I definitely don’t raise my two young sons this way.
As a mother and cook, I knew I needed to take a more modernized approach to feeding my family, which I refer to as the Clean Plate Club 2.0. We eat healthy, we eat clean, we don’t eat massive portions just because they are on our plates, and if you don’t like lima beans, by God, you don’t have to eat them!
Clean Plate Club 2.0
This is a great time to introduce the Clean Plate Club 2.0 concept to our followers, as it’s cervical cancer awareness month, which is top of mind for us here at Gennev.
Cervical cancer is highly preventable and treatable, provided that people take the steps to get screened and vaccinated. While the biggest risk factor for cervical cancer is an HPV infection, there are other health-related risk factors, including a diet low in fruits and vegetables and being overweight.
In 431 B.C., Hippocrates, the father of medicine, wisely said, “Let food be thy medicine and medicine be thy food.” We’ve all heard this before, but I always return to this quote as it is a reminder of the medicinal properties wholesome food can have on us. Now remember, in 431 B.C., people didn’t eat food out of boxes or wrappers, they ate fruits, veggies, whole grains and certainly weren’t eating foods that had been genetically modified!
So the Clean Plate Club 2.0 is loosely based on this revolutionary quote. As a nutrition coach, my mission is to educate you on the role that smart nutrition plays in nourishing your mind and body, and preventing illnesses like cancer.
I’m introducing Clean Plate Club 2.0 because studies have shown that you can fight cancer with food, particularly plant-based foods because they contain phytonutrients and other special compounds.
Participating in the Clean Plate Club 2.0 is easy. Here are three basic rules to follow:
One: Make veggies and leafy greens the stars of your plate at lunch and dinner.
Cruciferous vegetables like arugula, kale, cauliflower, Brussels sprouts and broccoli are low in calories, high in nutrients, and have sulfur-containing compounds with cancer-fighting properties. Opt to include two servings of veggies on your dinner plate with a small (optional) serving of whole grains and a small serving (4 oz or less) of lean protein.
Two: Minimize the number of added ingredients in your meals like sugar, dressings and mayonnaise.
Instead, add flavor to your dishes with real ingredients: healthy fats such as olive oil, avocado, Greek yogurt, lemon/lime juice and zest and spices like turmeric, cinnamon, ginger and curcumin, known for their anti-inflammatory properties. For example, make a quick and easy salad dressing with olive oil, lemon juice and curcumin instead of pouring a calorie-dense, preservative-laden bottled dressing onto your next salad.
Three: Reduce the amount of animal fat in your diet.
Meat, cheese, and butter can be rich in saturated fat, which has been linked to obesity “ a big cancer predictor. Look at these products as a treat, and a special accessory to your plate when you have them. If you are going to eat animal fat, splurge on organic, grass-fed meat and butter and sprinkle cheese onto foods sparingly.
The benefits of joining the Clean Plate Club 2.0 are numerous, but like anything else, you need to be consistent 95 percent of the time to see results. In addition to combating cancer, you’ll increase your energy levels, improve digestion and gut health, enjoy a clear complexion and feel lean and strong.
Open enrollment starts today, and I can’t think of a single reason that you shouldn’t join, but the main reason you should: because YOU are worth it.
Cheers to your health,
Michelle
How do you handle nutrition in your house? We’d love to know more as share with the community in the comments below, or hit us up on Facebook or Midlife & Menopause Solutions, Gennev’s closed Facebook group.
Gout? Isn’t that something men suffer from? Do woman get gout?
It is. And more and more women are getting diagnosed with gout as well.
In the last 20 years, cases of women with gout have more than doubled. According to the Arthritis Foundation, “…Two million women as and 6 million men as in the U.S. have this inflammatory form of arthritis that causes joint swelling and telltale pain at the base of the big toe.”
What is gout?
Gout is, as noted, a form of arthritis. Gout occurs when high levels of uric acid increase in the blood and form needle-shaped urate crystals in the joints or a joint’s surrounding tissue.
How does uric acid get produced?
When your body breaks down purines “ naturally-occurring substances in your body and in some foods “ uric acid is produced. The normal function includes this uric acid being dissolved in the blood, transferring to the kidneys, and then getting eliminated through your urine.
The body could be out of balance and develop gout by producing too much uric acid, or by excreting too little of it in the urine.
What does gout feel like?
A flare-up can swell the joints making it painful to walk or move, and can increase stress and frustration levels, which may then exacerbate other menopause symptoms like insomnia, night sweats, hot flashes, etc. Definitely not the direction to head in if you can possibly avoid it.
Joints may also swell, radiate heat, and flush red in color as well. A gout flare-up may also feel as though a joint is on “on fire,” like a joint-specific, localized hot flash of sorts.
If left untreated, gout pain may worsen and joint damage could ensue. Best to get it checked.
Is gout hereditary? If your family history includes gout, The Mayo Clinic notes you’re more likely to develop this disease.
In men, gout is often described as a sudden, severe attack, usually in the night, with intense pain in one of the joints, commonly the big toe. But this isn’t always the case with women.
In women, it can be a sudden attack, but it may also develop more slowly over time and in multiple joints. Brian F. Mandell, MD, a rheumatologist at the Cleveland Clinic in Ohio and board member of The Gout & Uric Acid Education Society, shares:
“In women, it seems there is a greater prevalence of the initial episode of gout being in multiple joints. It may not always be the typical swollen great toe. In the hands, this is often misdiagnosed as inflammatory osteoarthritis when it may actually be attacks of gout.”
Women frequently experience gout in the ends of their fingers, wrists, knees, and toes and are more prone to gout after menopause.
Ready to focus on your health in midlife and menopause? Work with a Gennev Menopause Health Coach.
Gout in women. What’s estrogen got to do with gout?
Estrogen in premenopausal women and those on estrogen replacement therapy helps to flush the uric acid out of the system, according to the Arthritis Foundation. After menopause, uric acid levels tend to rise.
If a person with a uterus develops gout before going through menopause, it’s usually due to other conditions such as having a history of taking diuretics, high blood pressure, diabetes, kidney disease, and obesity.
What about nutrition? Can diet manage gout and minimize flare-ups?
When it comes to diet, gout, and overall health, definitely get into your doctor’s office to talk about your health specifically. Especially if you have other health conditions.
Foods to avoid, limit, or moderate regarding gout
Some of the foods recommended to moderate or minimize may have health benefits that outweigh the risk for gout (like the omega 3s in sardines may be more important to brain health than sardines’ risk of gout). Knowing your levels, getting screenings, and having regular conversations about your health with your doctor or nutritionist will be your best way forward.
- Avoid gland or organ meats such as liver, kidney, and sweetbreads.
- Limit serving sizes of beef, lamb, and pork.
- Note and understand that some seafood including anchovies, shellfish, sardines, and tuna do have higher purine levels than other kinds of seafood.
- Limit or avoid sugar-sweetened foods (cereals, baked goods, candies, even some salad dressings), and limit the consumption of naturally-sweetened juices, like fresh-squeezed fruit juices.
On alcohol and gout
The topic offoods to avoid in menopause like alcohol comes up regularly in our content since it can spike the intensity and frequency of symptoms such as”¦ hot flashes, headaches or migraines, and mood swings (well, rage, really). It’s especially important to note for those prone to developing or who are actively managing gout.
Researchers out of the Boston University School of Medicine examined data on 2,476 female and 1,951 male participants in the ongoing Framingham Heart Study, which has followed residents of Framingham, Massachusetts, since the late 1940s. Over an average of three decades of follow-up, 304 cases of gout were reported, with one-third of those cases occurring in women.
Further reporting from the Framingham Heart Study shared that:
“Drinking 7 or more ounces of spirits a week — roughly five drinks — doubled the gout risk in men and tripled it in women. Heavy beer drinking was associated with a doubling of risk among men and a sevenfold increase in risk among women.” [emphasis ours]
Foods to include
We recommend weight loss,if you need it, for healthy menopause weight management. “Being overweight increases the risk of developing gout, and losing weight lowers the risk of it. Research suggests that reducing the number of calories and losing weight “ even without a purine-restricted diet “ lower uric acid levels and reduce the number of gout attacks. Losing weight also lessens the overall stress on joints.”
Recommended eats & drinks:
- Complex carbs. Eat more fruits, vegetables, and whole grains. Avoid foods and beverages with high-fructose corn syrup, and limit consumption of naturally sweet fruit juices.
- Water. Stay well-hydrated in menopause by drinking water.
- Fats. Skip or cut back on saturated fats from red meat, fatty poultry, and high-fat dairy products.
- Proteins. Focus on lean meat and poultry, low-fat dairy, and lentils as sources of protein.
Talk with your doctor, or one of our doctors, and your menopause health coach, about specific concerns about gout, joint pain, and other forms of arthritis. Talk with them sooner rather than later if obesity, high blood pressure, diabetes figures into your current state of health and well being.
Your health, mobility, and well being are worth it.
Join the Gennev Community Forums to weigh in on this topic, ask questions, and understand more about menopause with others on the path.
Shakespeare once described sleep as the “Chief nourisher in life’s feast.” Like good food, good sleep is vital to be nourished and healthy. If you’re going hungry, so to speak, the downstream effects poor sleep has on your body and spirit can be devastating.
For women experiencing hormonal changes, sleep is even more important “¦ and often more elusive.
Because sleep is so critical to our well-being, we asked our awesome physical therapists, Bri and Meagan, to help us understand why sleep is often interrupted and what we can do about it.
Why is sleep so important?
When the body is at rest, we’re regulated by the parasympathetic nervous system, says our PTs; this is the “rest and digest” system that calms the body, decreases heart rate, relaxes muscles, and allows us to digest our food and restore our bodies to their factory settings.
When we don’t get adequate rest, a whole chain of negative effects can follow, including:
- Compromised immune system. If you’re not getting enough sleep, you may find you get sick more often.
- Inflammation. Poor sleep increases cortisol levels, Bri says; and that can increase inflammation throughout our entire system. If we constantly have elevated levels of cortisol, our sleep never gets to those baseline resting levels where the body benefits most. As Meagan says, for their patients with pelvic pain, staying chemically wound up from elevated cortisol can increase pain and impact gastrointestinal and genital-urinary systems. When those systems are inflamed, we end up getting up more often in the night to pee, further disrupting our sleep.
- Reliance on sleep surrogates. It’s a bad cycle to get into: when we don’t sleep well, we tend to rely on caffeine or sugary drinks to keep us going. Unfortunately, those choices are irritants that can get us into the vicious cycle of urgency that results in painful urination that ends up causing more inflammation.
- Increased risk of disease, stress, and anxiety. Says Bri, if you’re not getting enough sleep, your parasympathetic system can’t do its job well, you’re not getting the restoration of tissue or the good blood flow your body needs to recover from the day. Those who don’t sleep enough may be at greater risk of depression, hypertension, diabetes, and digestive issues, among other concerns.
What will I really gain from getting more sleep?
So yeah, you can avoid all that bad stuff, but what good stuff do you get?
How about reduced pain? “When you have repeated nights of poor sleep, your senses get revved up,” Meagan says. “Pain that’s just a whisper now gets a little louder after one bad night, but after a week or a month of not enough sleep, that whisper is at a screaming-through-a-megaphone level of magnitude. Your neurological system can’t cope, it’s now a physiological problem. Once you start sleeping again, the pain loses volume, becomes a whisper again, and now you can ignore it and get back to a regular sleep cycle and a less-painful life.”
“She got two good nights in a row,
and her pain went from 8 out of 10 to a 4.”
One of Bri’s patients was in post-operation recovery and feeling considerable pain. “She got two good nights in a row, and her pain went from 8 out of 10 to a 4. It’s amazing what restful sleep can do for your body. As a healing mechanism, sleep is absolutely vital, but we underestimate how important and effective it is.”
Another benefit: better emotional health. There’s a good cycle and a bad one, our PTs note: “Poor sleep results in poor eating habits because you want sugar and carbs for energy.” Bri says. “You want to be active, but your workouts are compromised because you’re tired and eating a bad diet. So you do less because you’re tired, which leads to declining health, which leads to feeling unhappy with yourself. And that extra anxiety further interrupts your sleep. Sometimes all you need to break out of that cycle is sleep.”
Good sleep supports better overall health. As PTs, Meagan and Bri are often involved in helping patients reduce pain so they can sleep better. “We help with pelvic pain, with fluid intake and timing so our patients get better sleep. That creates a positive ripple effect that leads to better food choices, better activity tolerance because they have more energy, better exercise, better health. We’ve taken out their coffee after dinner and addressed pelvic floor spasms, so now they can sleep longer and deeper and begin to heal.”
Sold. How do I sleep better?
Because sleep is involuntary, we tend to assume we have little to no control over it. But there are things we can do to promote better sleep.
According to Meagan, having good sleep hygiene is really important. Create a routine and keep to it every night, even on weekends. Do the same things, in the same order, and as close to the same time every night as is possible.
Adjust your fluid intake to promote uninterrupted sleep as no caffeine in the evenings, reduce fluid intake in the time just before bed.
Turn off devices that create a stimulating light (cell phones, tables, laptops, televisions) early enough to reduce the impact on your nervous system. “Lots of people take their screens to bed with them,” says Bri. “We don’t want to miss out on what’s happening in our social networks. But it’s important to remember the bedroom is for sleeping and sex, not tweeting or TV, so turn off your screens sooner in the evening to unwind in time for bed.”
Kegel breathing is a technique our PTs use with patients: by coordinating the pelvic floor with breathing, you stimulate the parasympathetic nervous system, which promotes rest. Plus, says Meagan, “it gets mentally boring, so you can count Kegels like sheep until you drift off!”
Tip for better sleep: do Kegels
and count the repetitions like sheep.
Prioritize sleep. Women in particular, and even more, moms, tend to prioritize other things, says Meagan. We think we have to get things done, be productive, clean the house, catch up on work. “But when you start chipping away at sleep, the quality of all your other work gets compromised. If you get one more hour of good rest a night, it’ll take you so much less time to do those other things. And you’ll feel better doing them! Shift your to-do list to make sleep a priority.” Try things like weighted blankets to spice up your sleep routine, and make you more excited for sleep.
In our hyper-productive culture, sleep can feel like a waste of time or worse, like weakness. “Fess up: how often has someone called you and woken you up, and you lied and said you weren’t sleeping? How often do you hear people bragging about how little sleep they get? But the truth is, sleep is nourishment, and without enough of it, our bodies, minds, and spirits are far less healthy than they could be. Sleep truly is the chief nourisher in life’s feast as dig in!
We hear it a lot, and it’s a legitimate concern: science and medicine aren’t doing enough to help women, particularly women in midlife and menopause.
Well, times are changing.
Innovation around menopause care is happening, often at organizations led by women.
We’re truly excited to tell you that Gennev is partnering with one such innovative organization as MiraKind. Their research into the intersection of genetics, development of cancer, and menopause has revealed an exciting path for exploration and hope for women at high risk of certain kinds of cancer.
We talked with Dr. Joanne Weidhaas, MD, PhD and founder of non-profit MiraKind, about the KRAS variant she discovered, what her research means for women, and how she’s achieving her desire to bring doctors, patients, and scientists together for the benefit of all.
Can you explain what MiraKind is and what you do?
Dr. Joanne: MiraKind was founded in 2013, as a spin out from MiraDx, a company built on the discovery of a very new kind of cancer-associated genetic mutation. The purpose of MiraKind has been to share information about these mutations to the people they can help the most. Right now that is for women, as their first mutation, the KRAS-variant, predicts an increased risk of cancer.
Another priority of MiraKind is to help find prevention strategies for patients with the mutations they have discovered. For patients with the KRAS-variant, this strategy is to avoid estrogen withdrawal.
On your website, it says you engage in “patient-centric research.” What is that?
Dr. Joanne: At MiraKind, working hand-in-hand with the patient through direct patient contact and input is really a cornerstone of our philosophy. We want to learn from the patient as much as we want to educate them about our mutations and what they mean. We can’t find answers without them. And our goal is to find answers for them. Thus, it is really a two-way street!
So tell us about KRAS as what is it?
Dr. Joanne: Well, KRAS is a protein, and it is really important in cancer development, and treatment resistance. The KRAS-variant is the mutation that we discovered, which is basically the control knob for the KRAS protein. In people with the KRAS-variant, they do not control KRAS like other people. The communication between the regulators in the cell (micro RNA’s) and KRAS is flawed. So when non-KRAS-variant people lose estrogen, their cells stop growing; in those with the KRAS variant, cells start to grow, for example.
In some aspects of life, this probably makes them stronger, but, in certain situations, like hormone withdrawal, there is a miscommunication because of this different control knob, and they can develop cancer. The KRAS-variant is the very first example of a mutation of its kind in cancer. It is fundamentally different than other mutations associated with cancer, as we think we really can control it!
Should everyone get tested for it?
Dr. Joanne: Gosh, yes. we certainly think so! Absolutely all women when they become peri-menopausal at a minimum. It is so easy to be tested, and it is such important information to have when you are going through decisions about your health, from hormone replacement therapy, to screening! Because you can inherit the KRAS-variant from your dad, and cancer happens later, you do not need a strong family history of cancer to have the KRAS-variant.
Why is it particularly useful for women to get tested?
Dr. Joanne: As mentioned earlier, women are at a higher risk of developing cancer than men with the KRAS-variant. We have found that declining estrogen levels seem to be a main trigger for their cancer; thus, maintaining hormone levels is a really easy option to help prevent it.
How can I get tested?
Dr. Joanne: You can get tested by visiting our website at MiraKind.org, selecting the KRAS-variant test, and placing your order. We will send you a simple at-home cheek swab to obtain your KRAS-variant results, which we can share through a doctor of your choice, and ideally through the network at Gennev! The cost of testing is $295. You can also join a study through MiraKind.org and get a discount.
If I test positive for the variant, what’s my next step?
Dr. Joanne: The most important thing is to team up with a doctor who understands the KRAS-variant and is there to support you. The general recommendation is to continue estrogen and have that carefully managed. Also to get routine screenings, especially of the breasts and the ovaries.
What is the role for HRT in this conversation?
Dr. Joanne: Since we have found that declining estrogen levels trigger cancer in KRAS-variant positive women, we know that estrogen is protective for them. We support HRT, particularly in women with the KRAS-variant, as it helps protect them against their cancer risk.
Does HRT help prevent ovarian or lung cancer as well?
Dr. Joanne: We believe it will protect against all cancers in KRAS-variant women.
Why am I just now hearing about this very important research?
Dr. Joanne: There are a couple of reasons. First, this important research is really very new, and is such a paradigm shift. We now know that there are mutations that are control knobs, that they can be triggered (and thus managed), by external factors like estrogen, and that they can be as common as the KRAS-variant is. It’s very new, so we’ve chosen to develop this slowly and responsibly. Also, we wanted to find solutions, and not just scare people. We have chosen to do this through a non-profit model because we want to partner with patients to find prevention strategies. For us, prevention is the ultimate goal.
Where can I learn more?
Dr. Joanne: Visit us at our website at MiraKind.org or follow us on Facebook or Twitter @Mira_Kind. You can also just email me at joanne@mirakind.org!
Are you working on other genetic research?
Dr. Joanne: We have spent the last 10 years proving that the KRAS-variant is the incredibly powerful mutation that it is and finding other mutations like it. We now know exactly how to treat people with the KRAS-variant if they do develop cancer. We also can predict which patients will have toxicity to certain cancer treatments, like immune therapy, and radiation therapy. While the work on directing cancer treatment is done through our sister CLIA lab, MiraDx, the common theme to all of our work is to improve how we care for people and patients.
What is your role now, as head of MiraKind? What’s next for you and your organization?
Dr. Joanne: I also work as a radiation oncologist and vice-chair at UCLA, where I see breast cancer patients and run an R01 funded laboratory. I oversee the work that is done at MiraDx. I have always felt that MiraKind is where the heart of it all is. The ultimate goal for me is to empower people to get the necessary information to protect themselves from ever developing cancer. So the next steps are for us to find like-minded partners to help us do this!
At Gennev, we’re very excited to be able to help Dr. Joanne and MiraKind spread the word and get more women tested. If you think you may be a good candidate for the test or to help MiraKind in their research, we urge you to go to the MiraKind website to learn more and get started.
Have you been tested? Would you consider it? We’d love to know your thoughts on testing for genetic risk factors such as the KRAS variant. Please share with us in the comments below, join our community forums, tell us on Facebook, or join our closed Facebook group, Midlife & Menopause Solutions.
How many of you read The New York Times article What if Menopause Wasn’t Dreaded?
It was an opinion piece on Sept 12, 2019 by University of Georgia distinguished research professor Susan Mattern.
In it, she shares a history of menopause and takes us back to a time when it was named. She writes, “The word “menopause’ itself was coined by a French physician in 1821; by then, there were colloquial expressions for it in Europe, such as “women’s hell.'”
She plants a notion in readers’ minds that society sort of created the bad energy that menopause is associated with.
In the article she states, “This bleak view of menopause is unique to modernized cultures. In cultures with minimal exposure to modernization “ few of which survive today “ the idea that the end of a woman’s reproductive years will be accompanied by a collection of unpleasant symptoms (what physicians sometimes call “menopausal syndrome’) is hard to find. Hmong immigrants to Australia, for example, when questioned by researchers in the 1990s, were surprised to learn that white Australian women thought that menopause caused physical symptoms and problems.”
How profound. If we didn’t have awareness that menopause was a bad thing, would we even think that it was when it arrived? Or dread its natural cycle in our bodies?
There’s a fair amount of you reading this article who would loudly answer my question with a definite NO.
The symptoms are real. In fact, today I heard from a woman who told me every time she gets up on stage, she gets a hot flash. Another mentioned in a quiet voice that she now knows what other women mean when they say they “can’t control their anger.”
I, for one, believe menopause is very real. But I also believe that the social picture that’s been painted since the 1800s in modern cultures has unfairly flavored its role in our lives as women.
I wish we could reverse that. I wish we could see the transition in life through menopause as a preparation for the second half of life. And if we treat it with the care it deserves, our bodies, hearts and minds will be ready to lead our families, local communities, companies and organizations with only the wisdom that time on this planet can bring.
My wish is that when women (and men) think of menopause, they consider it the moment when women are preparing to “arrive.”
“I’ve arrived and I want everyone to know it” is the bumper sticker I’d like to print for all menopausal women.
Is this too far-fetched to even wish for? I believe we can start working to make this ginormous shift. You with me?
I’m encouraged by Professor Mattern’s view on menopause, because it’s not like we’re inventing anything new. We’re just making the old cool again.
We doubt that too many women actually look forward to menopause (though we happen to think it’s not a bad idea to start doing so!). Some of the symptoms of menopause you may encounter are: trying to get rid of hot sweats (and cold chills flashes), insomnia, irritability, and weight gain.
Unfortunately, hormonal weight gain symptoms in menopause aren’t the same as other types of weight gain, and can make it harder to lose the excess weight.
Discover what types of symptoms you should be on the lookout for and a few self-care tips to get you past the hormonal weight gain hump.
Common hormonal weight gain symptoms during menopause
The symptoms of hormonal weight gain during menopause are similar to the symptoms of other types of weight gain, which means this type of weight gain isn’t always easy to diagnose. Some common symptoms of hormonal weight gain include:
- Increased stress
- Insomnia or decreased sleep
- Binge eating/stress eating
- Fatigue and sluggishness
- Increased breakouts (blemishes/blackheads) on the chin
- Decreased estrogen levels
How do I know it’s hormonal weight gain?
In this case, the diagnosis is similar to the treatment – look at the hormonal weight gain symptoms above and ask yourself if you need to employ any of the tips included below.
Are you getting seven-to-nine hours of sleep each night? Do you wake feeling rested? Are you suffering from symptoms of menopause? How do you manage stress? Do you make exercise and healthy eating a priority?
If you need to up your emotional self-care routine and/or are experiencing other symptoms of menopause, your weight gain might be linked to hormonal imbalances.
Curbing hormonal weight gain symptoms during menopause
The number one thing you can do to curb hormonal weight gain (from both prevention and maintenance perspectives) is to up your self-care game. Since hormonal weight gain during menopause is much different from gaining a few pounds over the holidays, you’ll need to concentrate on hormone-related factors.
Self-care tip #1: exercise
Yes, this is what we would suggest if your weight gain wasn’t related to hormones, but we also feel that it’s worth mentioning for menopause-related weight gain too.
One of the best ways to regulate your hormones is to excercise. It helps your body produce endorphins, which are hormones that regulate mood and stress “ specifically, they can lower your stress and boost your mood.
But whatever you do, don’t overdo it with exercise. Overexercising can disrupt your hormones even further.
Self-care tip #2: eat for your hormones
What we put into our bodies plays a huge role when it comes to hormone regulation and weight management. When we eat foods that help regulate our hormones, we’re supporting our own bodies.
But if we consistently eat foods that disrupt our hormones and throw us out of whack, we might be facing even more weight gain.
Focus on whole foods, including a variety of veggies and fruits. Avoid any animal products that might contain growth hormones (or any other hormones for that matter!). Buy organic produce to avoid pesticides and wash your produce thoroughly before eating it. If you’re using plastics, always opt for BPA-free.
Caffeine, some food preservatives and Sugar can affect your hormones. Some women are also sensitive to dairy and soy. Try to eat these products carefully and sparingly. Though we won’t ever fault you for indulging here and there “ especially during the holidays!
Self-care tip #3: make sleep a priority
One of the biggest factors in weight gain (and loss) is sleep. If you don’t get enough shut-eye each night, it can be even harder for your body to shed those pounds or keep them off. (Read our tips on how to get better sleep during menopause!)
Researchers believe that you need somewhere between seven and nine hours of sleep per night. Getting less sleep than you need? Your metabolism could suffer. Some studies have even shown that cutting back on sleep can affect weight loss up to 55 percent “ without changing any food or exercise habits.
When you sleep, your body makes a hormone called leptin that can suppress hunger. When you don’t get enough sleep, your body instead makes a hormone called ghrelin, which can trigger hunger. This means that if you don’t get enough sleep, you’ll be hungrier than if you got a full eight hours.
Self-care tip #4: manage stress
Managing stress also plays a major role in weight management during menopause. This can happen in two ways.
One: Weight gain because of poor stress management – When we’re stressed, we tend to throw all self-care techniques out the door. It’s easier to reach for something unhealthy when we’re busy and stressed than take the time to make a healthy meal.
Many of us stress eat or binge eat when we’re under pressure. Yet, this is exactly what we shouldn’t do! Alcohol, sugar, salt, caffeine, and additives can negatively affect our stress hormones and make us feel even worse in the long-run “ even though that crunch or sugar fix seemed like a great short-term solution at the time.
Two: Weight gain because of stress hormones – We humans were built to survive. This means that we share many of the same traits as our prehistoric ancestors “ including fight-or-flight responses.
When our ancestors needed to run away from a threat (such as a predator), our hormones would kick into action, giving us stamina and strength to get away. Cut to today: when a debt collector sends a threatening email or letter, our bodies react as if the threat were more immediate and triggers our fight-or-flight responses.
Since we’re faced with stressors all day, every day, these stress hormones can send our bodies into overdrive. We don’t need these hormones to run away from debt collectors or texts from an ex; what we need is calm.
Sometimes managing stress can be just as stressful as the original stress itself. Luckily, there are a few tried-and-tested ways to keep stress at bay including:
- Taking a yoga or meditation class to help with menopausal moodswings.
- Downloading a mindful app
- Going for a walk
- Channeling your stress into a creative project or athletic activity
- Starting a gratitude journal
Self-care tip #5: love your body
No matter where you are physically or hormonally, it’s important to love your body just the way it is. Sometimes your weight will fluctuate — menopause or no menopause. There are often factors out of our control.
Maybe you just got back from vacation and saw the numbers on the scale inch up. We tend to eat comfort foods around the holidays. Maybe you just wanted to get a bowl of pasta at your favorite restaurant and now you’re holding water weight from all the sodium.
Whatever the reason for your weight gain, don’t let that number define you. Love your body “ all versions of your body “ and the number on the scale won’t matter as much anymore.
Learn more about hormonal weight gain
Combating Menopausal Weight Gain
Intermittent Fasting and Menopause
Belly Fat in Menopause: 5 Ways to Beat It
We can help you manage hormonal weight gain
- If you are can’t seem to lose those added hormonal pounds, a menopause-certified health coach can be helpful. We can create a personalized plan that fits your lifestyle. Book 30 minutes for your personal consultation with a health coach.
- Meet with a Gennev Doctor – our board-certified gynecologists specialize in menopause, and can help you understand your symptoms and create a customized treatment plan.
- Arm your body with our daily supplement specially formulated for women in menopause. Vitality supports mood, energy, stress response, immune health, joint pain, and inflammation.
The information on the Gennev site is never meant to replace the care of a qualified medical professional. Hormonal shifts throughout menopause can prompt a lot of changes in your body, and simply assuming something is “just menopause” can leave you vulnerable to other possible causes. Always consult with your physician or schedule an appointment with one of Gennev’s telemedicine doctors before beginning any new treatment or therapy.
by guest blogger Amanda Giralmo:
You’ve been hitting snooze on your alarm clock for days now like it’s the Staples Easy Button, but there’s nothing easy about dragging yourself out of bed when you’re feeling exhausted again. You somehow misplaced your keys in the fridge, and you feel overwhelmed by the fact that you should put something in your fridge other than your keys and four days’ worth of take out leftovers.
In short: you feel completely out of balance! But, how do you find this elusive balance that everyone is seeking in today’s always-on, go-go-go world?
Working with my clients as a holistic health coach, I can confirm that the struggle to feel mentally well and nourished physically, while also making sure those around you are cared for, is real!
In my practice, I work with smart, busy people who face this challenge often. My clients want to feel their best but aren’t quite sure how to get there on their own, so I create space and a supportive environment that enables them to articulate and achieve their wellness and lifestyle goals through actionable, bite-sized changes.
How to take care of yourself mentally
One of the tools I use to support my clients, and one of the ways I manage to keep my sanity, is by defining basic, self-care needs.
Self-care is all about nurturing and recharging yourself with the same kindness you provide to your loved ones. I may not complete a single one of my self-care needs in a day, but if a few days go by without including at least one, I feel my balance begin to tip. Here’s some insight into how I identified my self-care needs, so you can establish your own, and how to take care of yourself emotionally and physically.
Remove Guilt
The first step to defining your self-care needs is removing the guilt associated with taking care of yourself. Understanding your basic needs and showing yourself the love, respect and nurturing you deserve will allow you to sustain and find joy in caring for others. Removing guilt will help reduce your menopause anger attacks at yourself and others.
Stop Comparing
“Comparison is the thief of joy.”
“ Teddy Roosevelt
Do you have a case of “keeping up with the Joneses”? Like Teddy Roosevelt said, “Comparison is the thief of joy.” Skip to the beat of your own drum, by getting inquisitive with yourself:
- When do I feel most energized to complete big tasks?
- When and how often do I need quiet time alone?
- When and how often do I need to engage with friends, and how do I like to engage?
- What role does exercise play in my life?
Start designing your day around the answers to your personal Q&A and get your joy back.
I’ve learned that doing intense cardio workouts on a regular basis burns me out, even though I know numerous people who thrive on this type of exercise. I flourish when I have a mix of walking, yoga and strength training; these are a part of my weekly self-care basics. I’ve also found that focusing my social calendar on more intimate events that really allow me to connect with friends energizes me vs. attending large, crowded events. I tend to shy away from larger events, even though many of my friends enjoy them.
Sleep
Sleeping 8-9 hours per night is high up there for me in my basic self-care needs. The amount of sleep individuals need to feel rested can vary; however, most adults need an average of 7-8 hours of sleep per night.
Anyone looking to find balance in their life should get familiar with their sleep needs. Remove all tempting electronics from your bedroom, play around with different bedtimes, try waking up without an alarm clock a few days per week, until you find the good amount of sleep you thrive on.
Stress Busters
Deep belly breathing, meditation, nature walks, taking a technology time-out, calling a friend or loved one, taking a hot bath, watching a funny YouTube video can all help us relax. Play around with some or all of these, and pay attention to other activities that help to lower your stress.
The basic self-care needs that help me break through stress include daily meditation and time in nature (even if it’s just a walk around the block); weekly reiki, yoga and 1:1 time with my partner.
Infuse Delight
Playing is not just for kids; identify activities that bring you true delight! Traveling and experiencing new cultures make me feel like a kid on Christmas morning, so my yearly self-care includes at least two trips to somewhere new! Because I also enjoy new experiences, I’ve included new exercise classes, a guided meditation class, new hikes, dance lessons, and a shark dive at my local aquarium.
Once you have identified your self-care needs and their frequency, write them down, then spend a few minutes visualizing what life will be like when infused with these items. Identify the feelings associated with the visualization as relaxed, peaceful, energized, loving, etc”¦
When life starts to feel unbalanced, review what you wrote down and ask yourself as “when was the last time I did something to show myself love and support my basic needs?” Then choose one and go do it.
Gennev note: Certain content in this blog was inspired by content developed by Integrative Nutrition Inc. Integrative Nutrition Inc. does not endorse the content of this blog.